Retinopathy of prematurity is a vascular disease of the retina that develops in infants born prematurely. It involves the abnormal growth of retinal blood vessels and can lead to retinal detachment, resulting in complete and irreversible loss of vision.
Contact us and learn more about the available treatments of retinopathy of prematurity in Turkey!
We're Here to Help.
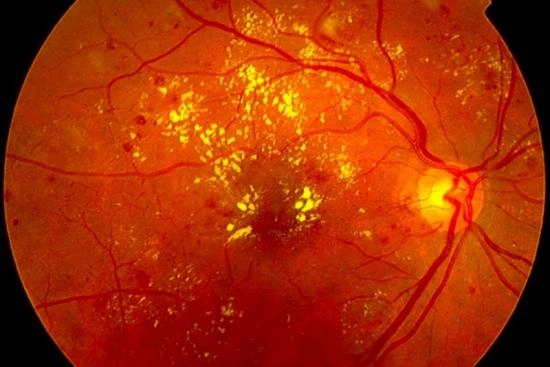
What is retinopathy of prematurity?
Retinopathy of prematurity (ROP),also called retrolental fibroplasia, is a disorder of the developing retinal blood vessels in premature infants.
The disease develops when the blood vessels grow unusually. It leads to the formation of a knot of tissue between the central retina and the peripheral retina. The risk of retinopathy of prematurity is closely related to the proportion of retinal surface area not vascularized at birth.
The chances of a newborn baby weighing less than 1 kg developing retinopathy are very high. Indeed, the disease occurs in 47 to 80% of cases where the infant weighs less than 1 kg. It can also increase in case of repeated clinical complications. A severe form of the disease manifests itself in 21-43% of these cases.
The different stages of retrolental fibroplasia
The classification of retinopathy of prematurity is done according to the stages of the disease as in the following table:
Stage 1 | Demarcation line. |
Stage 2 | A knot of tissue forms in the dividing line. |
Stage 3 | Extra-retinal fibrovascular multiplication. |
Stage 4 | Partial retinal detachment. |
Stage 5 | Total retinal detachment. |
What causes retinopathy of prematurity?
Retinopathy of prematurity depends on many causes and factors that increase the risk of its development. These disease-promoting factors are multiple, but there are two main ones:
Oxygen-dependent factors
Historically, the first risk factor for retinopathy that has been identified is poorly controlled oxygen therapy. Indeed, hyper-oxygenation of the retina of a newborn baby can cause retinopathy in premature babies. It causes damage caused by increased oxygen levels in addition to reduced levels of vascular growth factors.
Oxygen independent factors
In addition to oxygen therapy, other major risk factors for retinopathy of prematurity have been identified. These factors are:
- Low gestational age.
- Low birth weight.
- The quality of postnatal growth.
When and how should retinopathy of prematurity be diagnosed?
The retinopathy of prematurity develops between the 32nd and 34th weeks of gestation. So, the screening for the disease is usually done from the 31st week of gestation at birth. It is also performed in all newborns weighing less than 1.5 kg or who were born before 30 weeks of gestation.
The pediatricians diagnose the retinopathy of prematurity by a fundoscopic examination, also called an ophthalmoscopy. If the disease is detected, the examination may reveal two results:
- Benign case: A line of demarcation and a ridge.
- More serious case: Multiplication of the blood vessels of the retina.
Treatment of retinopathy of prematurity in Turkey
To combat retinopathy of prematurity, specialized ophthalmology clinics in Istanbul, Turkey, offer two main treatment options:
Laser photocoagulation
Laser photocoagulation is a treatment used in severe cases of retinopathy of prematurity. This treatment, which focuses on the avascular part of the retina, removes the peripheral retina. The goal is to reduce the incidence of retinal folds, retinal detachment, and the production of angiogenic growth factors.
It is necessary to monitor the retinal blood supply every 1 to 2 weeks until the blood vessels mature.
There are similar procedures, but they remain a last resort because they provide little benefit. One such procedure is vitrectomy with lens removal for childhood retinal detachment.
A newborn with a complete retinal detachment should be followed to diagnose the development of secondary glaucoma.
If the laser photocoagulation patient has residual scarring (scar tissue),he or she will need lifelong follow-up at least once a year.
Treatment with Bevacizumab
Bevacizumab is an anti-vascular endothelial growth factor monoclonal antibody. Treatment with this anti-growth factor is a recent advance in the fight against retinopathy of prematurity. It helps stop the progression of the disease in newborns.
Compared with laser therapy, bevacizumab has a lower recurrence rate and a lower prevalence of myopia.
Unfortunately, despite its advantages, anti-VEGF therapy remains a second-line treatment. This is due to the associated disadvantages, including
- Need for high doses of bevacizumab.
- Risk of infection.
There are other treatments for retinopathy of prematurity such as scleral buckling.
Cost of treating retinopathy of prematurity in Turkey
In addition to providing the right treatment for your children's health, our partner clinics in Turkey are internationally renowned. They offer the services of world-renowned doctors. In addition, professional and attentive hospital staff will make your stay easier.
Finally, our partner hospitals offer the most competitive prices available. The total cost of treatment for preamputeal retinopathy varies depending on the hospital and its location. However, the price remains lower than other European clinics, while maintaining the same quality of therapy.
To find out more about the details and cost of the surgery, fill out the form on our website and opt for a personalized quote.
Share this page
